Our NDIS Community Nursing Care Services Provider in Perth
- Wound Care and Dressings
- Continence Assessments (Adults and children>2yrs)
- Medication Management (Oral and HRMs-Insulin, Clexane)
- Enteral Feeding
- Catheter care (IDC, IMC, SPC)
- Bowel care

About Our NDIS Community Nursing Care Services
- We are Committed to wound care.
- We use evidence-based care to promote healing.
- We provide assessment on acute and chronic complex wounds that are not healing including :
- pressure injuries
- lower limb ulcers
- palliative wounds
- slow to heal wounds
- We review the best products for care with representatives.
- We provide wound management plan.

- Medication safety is part of National Safety and Quality Health Service standards (NSQHS) second edition in Australia.
- We follow the best practice of safe medication administration as per NSQHS standards on medication safety. There is no standard list of high-risk medications in Australia, and they may vary between hospitals and other health care settings.
- 8% of Australians >65yrs and over receive residential aged care each year and take up to 9 or more medications regularly.
- Risks of medication administration and adverse drug reactions always remain high.
| Antimicrobials |
Aminoglycosides: gentamicin, tobramycin, and amikacin vancomycin
amphotericin – liposomal formulation
|
| Potassium and other electrolytes |
Injections of concentrated electrolytes: potassium, magnesium, calcium, hypertonic sodium chloride
|
| Insulin |
All insulins
|
| Narcotics (opioids) and other sedatives |
hydromorphone, oxycodone, morphine, fentanyl, alfentanil, remifentanil and analgesic patches
Benzodiazepines: diazepam, midazolam thiopentone, propofol and other short-term anaesthetics
|
| Chemotherapeutic agents |
vincristine, methotrexate, etoposide, azathioprine
Oral chemotherapy
|
| Heparin and other anticoagulants |
Heparin and low molecular weight heparins (LMWH): dalteparin, enoxaparin
Warfarin
Direct oral anticoagulants (DOACs): dabigatran, rivaroxaban, apixaban
|
| Systems |
Medication safety systems such as independent double checks, safe administration of liquid medications, standardised order sets and medication charts etc
|

- Enteral feeding is also known as tube feeding. It’s a way of delivering nutrition directly to your mouth, oesophagus, stomach and/ small intestine.
- Enteral feeding may become necessary when you can’t eat enough calories to meet your nutrition needs or if you physically can’t eat due to various conditions leading to malnourishment, weight loss and very serious health issues.
- Cancers (neck, throat, stomach, intestine)
- Stroke and paralysis
- Other Neurological and muscular disorders like MS, Cerebral Palsy etc.
- Critical injury to vital organs.
- GI dysfunctions like Crohn’s disease, ulcerative colitis, bowel obstruction
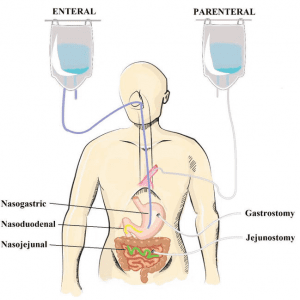
Types of Enteral Feeding include:
- Nasogastric tube (NGT) starts in the nose and ends in the stomach.
- Nasoenteric tube starts in the nose and ends in the intestines (subtypes include nasojejunal and nasoduodenal tubes e.g NJT).
- Oroenteric tube starts in the mouth and ends in the intestines.
- Gastrostomy tube is placed through the skin of the abdomen straight to the stomach (subtypes include PEG, PRG, and button tubes).
- Jejunostomy tube is placed through the skin of the abdomen straight into the intestines (subtypes include PEJ and PRJ tubes).
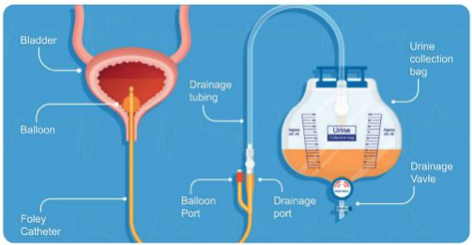
- If you have SPC (suprapubic) or IDC (indwelling) catheter, we will take care of its care and management.
- IMC is usually managed by yourself. We can give you education and training on do’s and don’ts with the catheter to avoid any infections like UTI’s.
- It is important to clean and care for your catheter to prevent any infections spread or complications such as blockage.
- Weak pelvic floor muscles
- Diarrhoea and bowel urgency
- Constipation
- Pregnancy
Why choose our Nursing Service?
- We provide person centred approach to all participants including CALD (culturally and linguistically diverse) communities by utilising TIS interpreter services to non-English speaking participants to help us understand their needs better.
- We are experienced- Our nurses have experience working across aged care, hospital, and community nursing areas.
- We have Immediate availability without any waitlist.
- We offer nursing service to all Perth metro areas specifically within NDIS range of 30min travel for ongoing nursing support based on participants NDIS funding. Please feel free to contact us to find out more about covering out of range areas for specific once off assessments e.g., continence assessments.
- We work flexibly and provide support afterhours/over weekends if required by participant based on their unique needs and NDIS plan budget.
Get in touch with us today and find out about the application and planning process.
Frequently Asked Questions
How do your community nurses coordinate with doctors and other healthcare providers?
Our community nurses often work closely with GPs, specialists, and allied health professionals, sharing updates and ensuring care plans are followed correctly.
Can your community nursing help prevent hospital readmissions?
Yes. Regular monitoring, medication management, and early detection of issues can significantly reduce the chances of returning to hospital.
What types of medical procedures can be done at home through your community nursing?
Our community nursing may include wound care, injections, catheter care, medication administration, vital monitoring, and chronic disease management.
Is your community nursing suitable for people with complex medical needs?
Absolutely. Our community nurses are trained to handle complex conditions, including high-care needs, palliative care, and chronic illness management.
How does your community nursing support family members or carers?
Our community nursing provides guidance, training, and relief for carers, helping them manage daily care tasks more confidently and reducing stress.
Can your community nurses assist with medication errors or confusion at home?
Yes. They help organise medications, ensure correct dosages, and educate patients to prevent mistakes and improve safety.
How often can your community nursing visits be scheduled?
Visit frequency depends on individual needs—it can range from daily visits to weekly check-ins or as required under a care plan.
What happens if my relative's condition suddenly changes during home care?
Our community nurses are trained to assess changes quickly, provide immediate care, and escalate to emergency services or doctors if needed.
Does your community nursing only focus on physical health?
No. It also supports emotional wellbeing by providing reassurance, building trust, and helping patients feel more comfortable and confident at home.






